Your 2026 Summer Skin Strategy: 5 Habits to Prevent Non-Melanoma Skin Cancer

Skin cancer continues to be the most common cancer diagnosis in the United States. For many, focusing on how to avoid skin cancer with hotter, sunnier days in the summer becomes a top priority. The good news: Your daily habits are your strongest defense against sun damage. In this blog, we’ll share the essential checklist […]
Basal Cell Carcinoma vs. Squamous Cell Carcinoma: What’s the Difference?

Melanoma and non-melanoma are two primary categories of skin cancer. Each presents different symptoms and treatment options. Within the non-melanoma skin cancer – sometimes referred to as NMSC – category, the two most common types are basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). While both are common forms of non-melanoma skin cancer, they […]
Keloids Treatment: What Options Are Available?
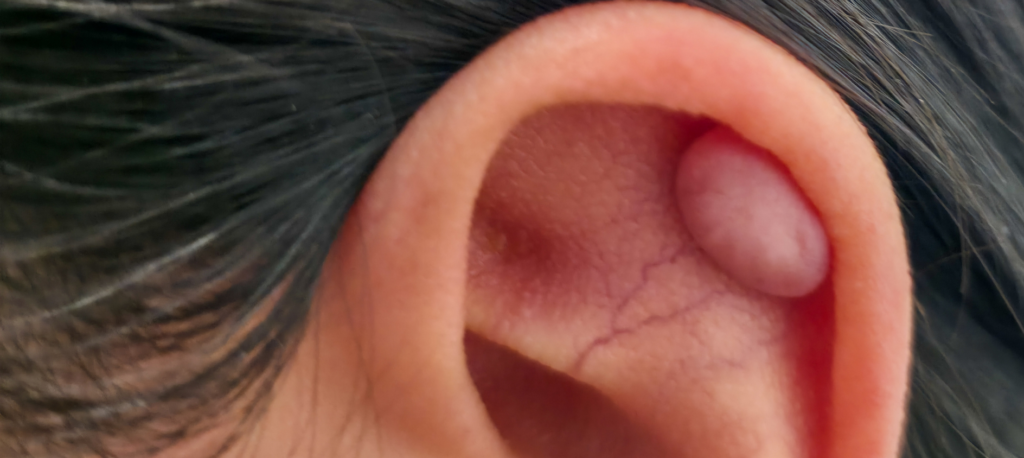
For the 10 percent of the population that suffers from keloids, finding an effective treatment option can often feel like a challenge. Traditional treatment options are limited in truly removing a keloid and keeping the keloid from forming again. Dr. Posten, board-certified dermatologist and Mohs surgeon at Advanced Dermatology Associates, frequently works with patients who […]
Innovation, Patient Outcomes, Collaboration: Key Trends Defining Dermatology in 2026

Thousands of dermatologists and industry experts attended the 2026 American Academy of Dermatology (AAD) Conference in Denver. As with previous years, it is the premier event for defining the next chapter of the specialty – and this year was no different. Our team at Sensus Healthcare was on the ground at AAD, collaborating and sharing […]
What is Keloid Disease?
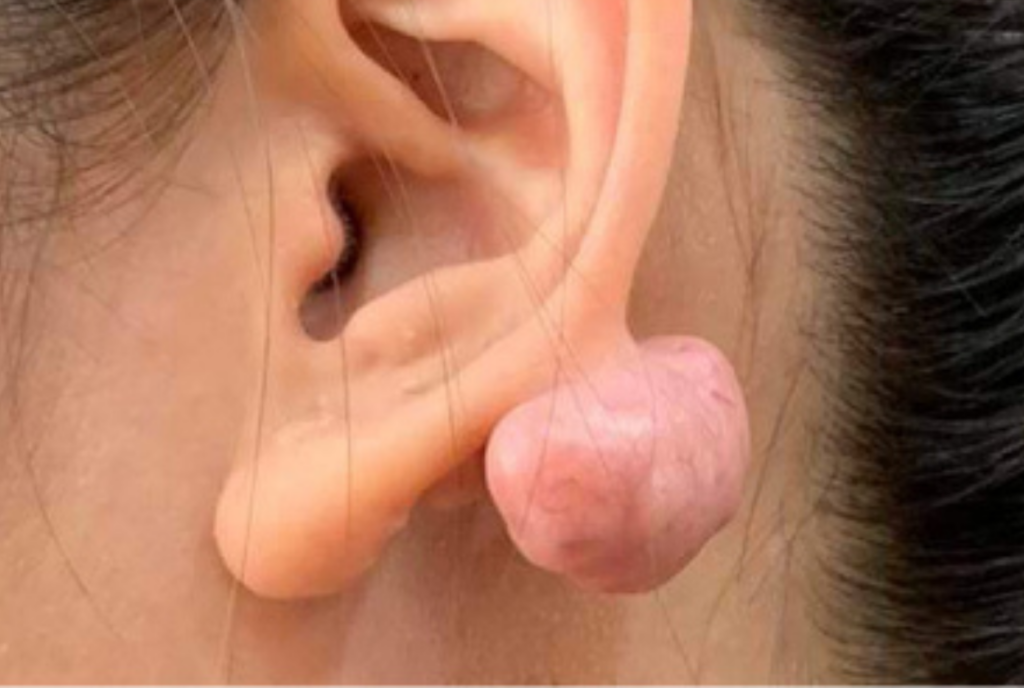
When you get a cut, a piercing, or even a bug bite, a scar can be a sign that our body is healing. But, for more than 150 million people around the world, what starts as a scar can grow into a skin condition known as keloid disease. By medical definition, keloids are overgrowth of […]
Beyond the Billing Code: What the New 2026 CMS Standards Mean for Non-Invasive Skin Cancer Treatment
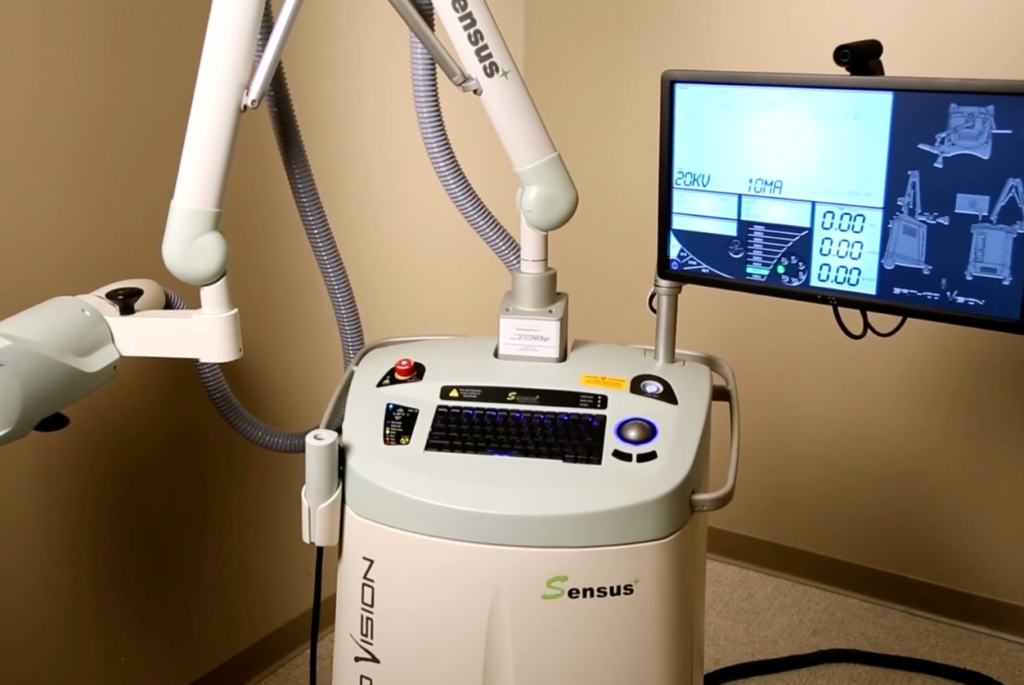
Skin cancer rates continue to increase, with the American Dermatology Association most recently estimating that one in five Americans will experience skin cancer in their lifetime. As skin cancer rates rise, so does the demand for non-invasive skin cancer treatment options. Superficial radiation (SRT) technology provides an alternative to traditional Mohs surgery, giving patients an […]
The Cost of Skin Cancer Treatment: What Non-Invasive Treatment Means for Healthcare

Skin cancer is the most common form of cancer in the United States. It is estimated that one in five Americans will have skin cancer before they reach the age of 70. With millions of new cases diagnosed each year, the cost of skin cancer treatment has become an important focus for many. Typical treatment includes Mohs surgery, […]
Understanding CMS Codes: How They Impact Your Reimbursement and Patient Care

For many healthcare providers, navigating CMS codes (Centers for Medicare & Medicaid Services codes) can feel like learning another language. Yet these codes are the foundation of proper billing, clean claims, accurate reimbursement, and patient access to care. As the healthcare landscape evolves, understanding how CMS codes function is essential for both administrative efficiency and […]
Treatment for Uncommon Skin Cancer Locations

When most people think of skin cancer, they imagine sun-damaged areas like the face, shoulders, or arms, but there are uncommon skin cancer locations that are often overlooked. Even when the summer is over, skin cancer is a year-round concern for all nooks and crannies of your body. Early detection is critical, and understanding the […]
Shifting the Standard: Why Non-Invasive Skin Cancer Treatments Are the Future of Skin Cancer Therapy

As October is Breast Cancer Awareness Month, a time dedicated to education, early detection, and advancing treatments that prioritize survival and quality of life, we are reminded how non-invasive skin cancer treatment is important in working towards the same goals of helping patients find treatment options that work for their unique lifestyles. This month provides […]


